When parents first hear that their baby has hypospadias, it can feel confusing or even frightening. The good news is that this condition is common, well-understood, and very treatable. With proper care from a pediatric urologist, most children go on to have a normal penile appearance and function.
Let’s break down what hypospadias is, what causes it, and how it’s managed — in simple terms.
What Is Hypospadias?
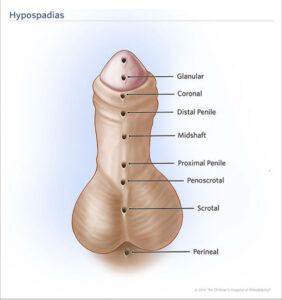 Hypospadias is a condition that affects the penis. In boys with hypospadias, the urethral opening (where urine comes out) is not located at the tip of the penis.
Hypospadias is a condition that affects the penis. In boys with hypospadias, the urethral opening (where urine comes out) is not located at the tip of the penis.
Instead, it can appear:
- Just below the tip (the most common type)
- Along the shaft
- Near the scrotum
In rare cases, even farther down.
| Type | Description | Frequency |
|---|---|---|
| Distal (glanular or coronal) | Opening near the head of the penis | Most common (70%) |
| Midshaft | Opening along the middle of the shaft | Moderate |
| Proximal (penoscrotal or scrotal) | Opening near or in the scrotum | Least common, more complex |
The severity of hypospadias depends on how far the urinary opening is from the tip of the penis and whether there is any significant curvature. Some boys also have a downward bend during erection, called chordee, and the foreskin may look incomplete or “hooded,” which is a common feature of this condition.
How Common Is It?
Hypospadias is one of the most common congenital (present at birth) conditions in boys, affecting about 1 in every 200–300 newborn males. It’s typically identified at birth during the baby’s first physical exam.
What Causes Hypospadias?
Hypospadias develops early in pregnancy — usually between 8 to 14 weeks of gestation, when the penis and urethra are forming.
The exact cause isn’t always clear, but several factors can play a role:
- Genetics: Hypospadias can run in families. If one boy is born with hypospadias, the chance of future male siblings having it is higher than in the general population. In addition, males with hypospadias have an increased likelihood of passing the condition on to their own children.
- Hormonal influences: Low androgen (male hormone) levels or tissue sensitivity during development.
- Environmental exposures: Certain maternal factors, such as hormonal treatments during pregnancy, may contribute.
- Prematurity or small size for gestational age can slightly increase risk.
It’s important to note that parents did not cause this — it happens naturally during fetal development and is not linked to anything they did or didn’t do.
How Is It Diagnosed?
Most cases of hypospadias are identified shortly after birth during the routine newborn exam. It’s often noticed when a family is considering a newborn circumcision, because hypospadias is a contraindication to circumcision. In these cases, a referral to a pediatric urologist is recommended.
A pediatric urologist may suggest additional evaluation if:
- The urinary opening is very low or there is significant curvature
- Other genital differences are present (such as undescended testicles)
- There is concern for a more complex disorder of sexual development (this is very rare)
Circumcision should be postponed until after a specialist evaluation, since the foreskin is often needed for the surgical repair.
Treatment: Surgical Repair
The main treatment for hypospadias is surgery, typically done between 6 and 18 months of age.
The goals of surgery are to:
- Move the urethral opening to the tip of the penis,
- Straighten any curvature (chordee),
- Reconstruct the foreskin or circumcise if preferred, and
- Create a natural appearance and function.
The procedure is done under general anesthesia, and most children go home the same day or after a short stay.
Recovery and Follow-Up
After surgery:
A small stent or catheter may be placed for several days to support healing. Whether a stent is needed depends on the severity of the hypospadias—the more proximal the opening, the more likely a stent will be used. Most stents remain in place for about 7 days and are removed in the office.
Parents will be taught how to care for the surgical site, keep the area clean, and reduce the risk of infection.
Pain after surgery is typically mild to moderate and responds well to medication. At OKC Kids Urology, we do not prescribe opioids for this procedure. Instead, discomfort and swelling are effectively managed with over-the-counter medications such as Tylenol and ibuprofen.
Follow-up visits usually occur about 1 month after surgery to assess healing, monitor urination and cosmetic results, and ensure the urethra continues to heal properly as the child grows.
Most children heal very well and urinate normally once the repair is complete. Long-term complications are uncommon but may include:
- Urinary spraying,
- Fistula (a small leak under the skin), or
- Scar tissue narrowing the urethra (stricture).
If these occur, your pediatric urologist can manage them with additional minor procedures.
Long-Term Outlook
With proper repair, children with hypospadias grow up to have:
- Normal urinary function
- Normal fertility potential
- Typical sexual function in adulthood.
Cosmetic outcomes are usually excellent, and most boys won’t even remember the surgery as they grow older.
Key Takeaways for Parents
- Hypospadias is common and correctable.
- Do not circumcise before seeing a pediatric urologist.
- Surgery is usually done between 6–18 months of age.
- Long-term results are typically excellent with normal function.
- Gentle reassurance and open discussion help families feel at ease throughout the process.
Final Thoughts
Hearing that your child has hypospadias can be overwhelming at first, but you’re not alone. Pediatric urologists perform this repair routinely with excellent outcomes. With early evaluation, skilled surgical care, and compassionate support, most boys recover beautifully and go on to live healthy, confident lives! Please don’t hesitate to reach out to OKC Kids Urology. We’re here to support you and your child every step of the way.
📞 405-286-0755